Jun 13, 2017
Singapore ranked fifth in a Philips survey on readiness to achieve a fully integrated health system
The first Future Health Index by Philips shows Singapore have better access to healthcare with aging population as number one challenge
Singapore – Royal Philips (NYSE: PHG, AEX: PHIA) today announced that Singapore received an overall score of 57.7 out of a possible 100 points, placing it fifth out of 13 in Philips’ first edition of its Future Health Index (FHI). The FHI explores how countries around the world are positioned to meet long-term global health challenges. Examining the perceptions, behaviors and attitudes of both patients and healthcare professionals, the Future Health Index focuses on three important factors necessary to move toward a more integrated system of healthcare: access to healthcare; integration of the current health system; and adoption of connected care technology.
The Future Health Index has uncovered significant insights into the key concerns of both patients and healthcare professionals in Singapore. In particular, the aging population emerged as a cause for concern among Singaporeans surveyed. Given this challenge, and consistent with other markets, the need for greater access to homecare resources and support is apparent,”
Fabian Wong
Chief Executive Office, Philips ASEAN Pacific
With a score of 57.7, Singapore is ranked fifth and ahead of the 13-country average of 56.5. The republic came in behind the United Arab Emirates, which achieved the highest score with 65.3, the Netherlands and China also coming in high, with scores of 58.9 and 58.1, respectively, and Australia with a slightly higher score of 57.9. Surprisingly, Germany, Brazil and Japan received the lowest scores in terms of readiness, at 54.5, 50.6 and 49.0, respectively. Three-quarters (76%) of healthcare professionals in developed markets agree their patients have access to the treatments needed for current and future medical conditions, versus just over half (58%) of those in emerging markets. In Singapore, this statistic was 86%, on par with Australia at 88%. While both patients (62%) and healthcare professionals (65%) agree that Singapore’s current health system meets the healthcare needs of patients, a key area of concern is the cost of healthcare. Results show a clear disconnect between costs versus value of healthcare received between patients and healthcare professionals. Patients (58%) believe that costs are too high for them relative to value, while healthcare professionals (51%) believe healthcare is priced about right. Patients and healthcare professionals agree the most important challenge in Singapore today is an aging population, at 58% and 78% respectively. This was ahead of other perceived key challenges. Patients and healthcare professionals ranked economic/financial problems second at 37% and 51% respectively. “While Singapore has done well in providing access to healthcare, we need to focus more on driving the integration of our health system and the adoption of connected care technology if we are to provide a healthcare system that is responsive to the modern and evolving needs of a growing, and aging population. Philips is committed to helping Singapore encourage its citizens to embrace technologies that empower them to better understand and thereafter take more active control of their own health,” added Mr Wong. Other key findings from the FHI study showed: Data sharing continues to be a challenge. Despite progress towards universal medical records in some markets, the vast majority of patients (74%) across all 13 countries surveyed report having to provide the same information to multiple healthcare professionals, and most (60%) have also experienced repeatedly taking the same medical tests. At the same time, even though more than half (60%) of patients in the 13-country total own or use a connected care technology to monitor various health indicators, only one third of these patients (33%) have ever shared this information with their healthcare professional. Across 13 countries, bureaucracy is seen as a major stumbling block. Over half (54%) of healthcare professionals and 43% of patients across the 13 countries surveyed indicate health system bureaucracy is a major barrier to further coordinating healthcare in their countries. While 45% of healthcare professionals in Singapore rate bureaucracy as a top barrier, 28% of patients say the same. However, it is important to note that 70% of healthcare professionals think the financial structure of Singapore’s health system would have a positive impact on the integration of health data. Who’s responsible for your health? Perception gaps also exist on the onus for preventing poor health. Across the 13 countries surveyed, as patients age, they are more likely to believe they are the guardians of their own health – 79% of those 55 years or older in the 13-country total agree the individual is fully responsible for preventing poor health compared to younger patients (66% of those aged 18-34 across 13 countries). While Singaporean patients across all age groups agree that it is the responsibility of the individual to prevent poor health, those aged between 55 and 64 take the lead in this category, with 84% believing the individual is fully responsible for their own health. Opportunity for Singapore patients to take more active control of their health management, which could be powered through greater adoption of connected care technology. Healthcare professionals in Singapore see a need for patients to increase their health management, as 60% say their patients need to take a more active role in managing their health. Compared to the 13-market average (56%), patients in Singapore are significantly less likely to say they actively manage their health (49%). Patients and healthcare professionals in Singapore believe in patients’ ability to manage their own health. Many patients and practitioners believe that patients have the knowledge (70% and 52% respectively), and tools (58% and 61%) to manage their own health. Across 13 countries surveyed, a clear majority of patients (69%) feel they have the knowledge to manage their own health effectively. However, less than half of practitioners (40%) agree. Cost of connected care technology is a key challenge. In Singapore, healthcare professionals and patients (61% and 66%) believe connected care technology would increase the cost of healthcare overall. This slightly exceeds the 13-country total findings (52% of healthcare professionals and 51% patients), which identifies key worries about resources needed for associated needs, such as training and data security contributing to overall concerns.
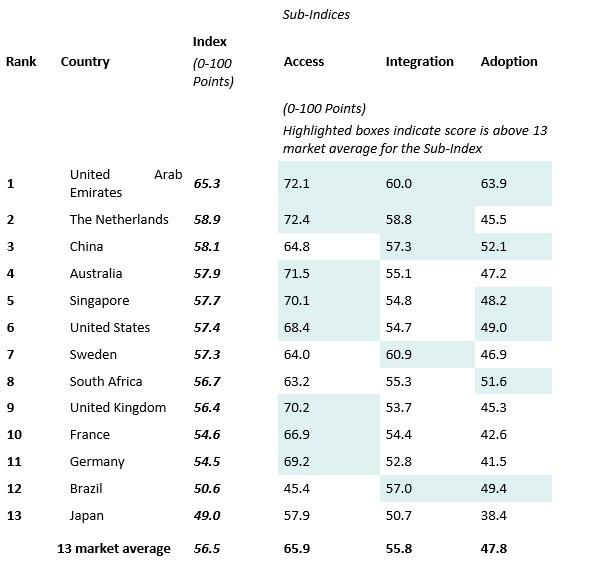
To read the Future Health Index report in its entirety, and to access local market data in-depth, please visit: www.futurehealthindex.com . Philips’ first edition of its Future Health Index explores how countries around the world are positioned to meet long-term global health challenges
About Royal Philips
Royal Philips (NYSE: PHG, AEX: PHIA) is a leading health technology company focused on improving people's health and enabling better outcomes across the health continuum from healthy living and prevention, to diagnosis, treatment and home care. Philips leverages advanced technology and deep clinical and consumer insights to deliver integrated solutions. Headquartered in the Netherlands, the company is a leader in diagnostic imaging, image-guided therapy, patient monitoring and health informatics, as well as in consumer health and home care. Philips' health technology portfolio generated 2016 sales of EUR 17.4 billion and employs approximately 70,000 employees with sales and services in more than 100 countries. News about Philips can be found at www.philips.com/newscenter.
About the Future Health Index
Philips undertook original research to understand the perception towards connected care and the role it plays in the future of healthcare. The study, which will be run annually, included both quantitative surveys and qualitative in-depth interviews. These were conducted from February-April, 2016 in 13 countries. A survey was fielded from February 24, 2016 to April 8, 2016 in Australia, Brazil, China, France, Germany, Japan, The Netherlands, Singapore, South Africa, Sweden, UAE, U.K. and U.S. in their native language. A combination of online, face-to-face (computer-assisted) and phone (computer-assisted) interviewing was used to reach a total sample of: At the 95% confidence level, the margin of error is +/- 2.2 percentage points for the Singapore sample of patients and an estimated +/- 6.9 percentage points for the Singapore sample of healthcare professionals. To provide context around the quantitative data, the survey was supplemented with 30-45 minute in-depth interviews conducted from March 7-April 11, 2016. The following audiences were interviewed in-person or over the phone: healthcare professionals (20 per market in all 13 markets); insurance professionals (8-10 per market in China, France, Japan, The Netherlands, UK, US); and public policymakers (8-10 per market in China, France, Japan, The Netherlands, UK, US). Secondary research was also conducted, gathering information from third party data and case studies to further validate the primary research results. The Future Health Index (FHI) is calculated by combining the quantitative survey responses from patients and healthcare professionals equally on questions about access to the healthcare system, their country’s current state of health integration and adoption of connected care technology and. The Index ranges from 0 to 100 points, and is the average of three sub-indices: access (across the health continuum); integration (of health system); and adoption (of connected care technology). Each of the three sub-indices range from 0 to 100 points, and each are weighted equally in the final FHI score. The three sub-indices scores are based on a series of question groupings (or components) that draw from a distinct theme in the questionnaire.
Topics
Contacts

Elaine Ng
Head of Communications
Philips ASEAN Pacific